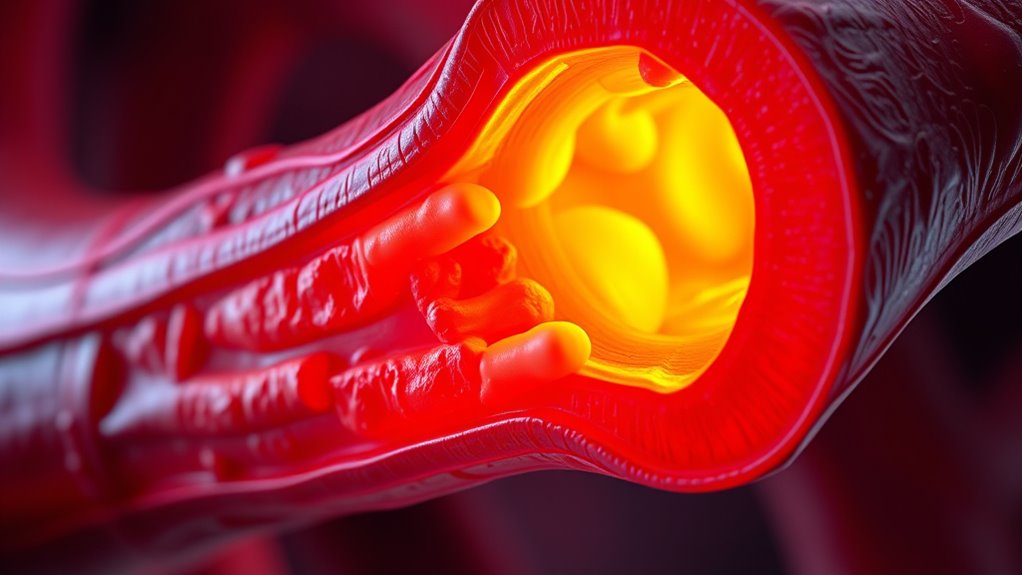
Hyperlipidemia means you have high levels of cholesterol and triglycerides, raising your risk of heart disease and stroke. You can manage it by adopting a heart-healthy diet, exercising regularly, and losing excess weight. Sometimes, lifestyle changes aren’t enough, and your doctor may recommend medications like statins. Understanding your genetic risk and combining these strategies can help control your levels better. Keep exploring to discover more ways to protect your heart health.
Key Takeaways
- Hyperlipidemia involves high LDL and low HDL cholesterol, increasing risk of heart disease and stroke.
- Genetics play a role; family history can predispose individuals to elevated lipid levels.
- Lifestyle modifications like a healthy diet, regular exercise, and weight management are essential for control.
- Medications such as statins may be prescribed when lifestyle changes are insufficient.
- Regular lipid monitoring and a holistic approach help prevent long-term cardiovascular complications.
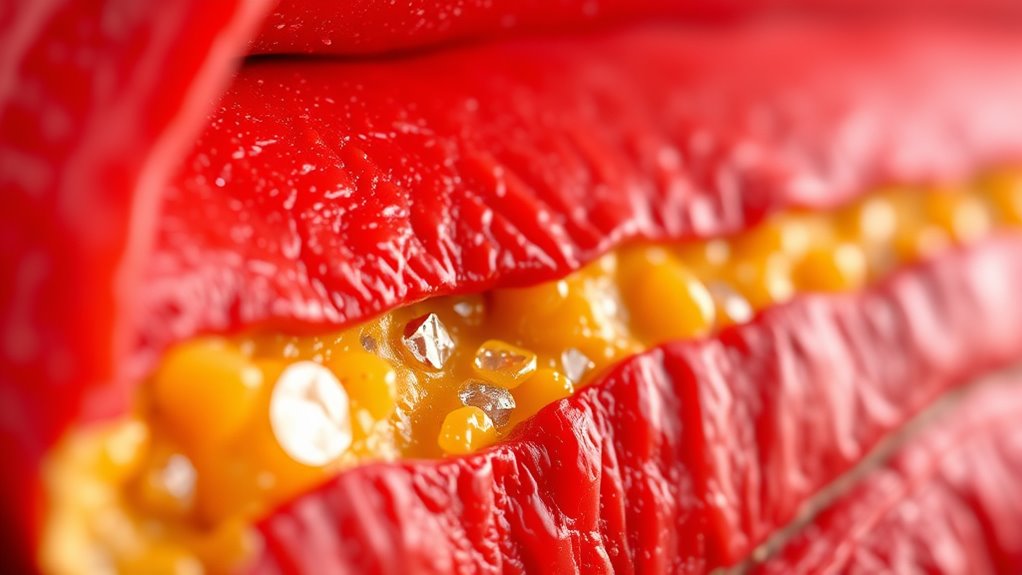
Hyperlipidemia, a condition characterized by elevated levels of lipids such as cholesterol and triglycerides in your blood, increases your risk of heart disease and stroke. Understanding the causes behind this condition can help you take effective steps to manage it. One major factor influencing hyperlipidemia is genetics. If your family has a history of high cholesterol or heart disease, you might be more predisposed to developing high lipid levels yourself. Genetic factors can affect how your body processes and clears lipids, making some individuals more prone to lipid buildup regardless of lifestyle. Recognizing your family history encourages you to monitor your lipid levels regularly and work closely with your healthcare provider to develop a tailored management plan.
Genetics influence hyperlipidemia; family history warrants regular lipid monitoring and personalized management.
Alongside genetics, lifestyle modifications play a vital role in controlling hyperlipidemia. You have the power to make changes that considerably reduce your risk. For starters, adopting a heart-healthy diet can make a big difference. Focus on reducing saturated fats found in red meats and full-fat dairy, and avoid trans fats often present in processed foods. Incorporate more fruits, vegetables, whole grains, and sources of healthy fats like nuts, seeds, and oily fish, which contain omega-3 fatty acids. These dietary adjustments can help lower your LDL cholesterol—the “bad” cholesterol—and raise your HDL cholesterol—the “good” cholesterol.
Physical activity also contributes notably to managing lipid levels. Regular exercise, such as brisk walking, cycling, or swimming, can help you boost HDL levels and lower triglycerides. Aim for at least 150 minutes of moderate-intensity activity each week. If you’re overweight or obese, losing even a few pounds can improve your lipid profile and lessen your overall cardiovascular risk. Besides diet and exercise, quitting smoking and limiting alcohol intake are essential lifestyle modifications. Smoking damages your blood vessels and lowers HDL cholesterol, while excessive alcohol consumption can raise triglyceride levels.
In addition, understanding how synthetic wigs are styled can help you achieve a festive look for Halloween or other occasions. Medication may be necessary if lifestyle changes aren’t enough to bring your lipid levels into a healthy range, especially if you have a strong genetic predisposition. Your doctor might prescribe statins or other lipid-lowering medications to help manage your condition effectively. However, these medications work best when combined with ongoing lifestyle modifications. Staying informed about your genetic risks and actively making healthier choices empower you to control hyperlipidemia and protect your heart health over the long term. Remember, managing your lipids isn’t just about medication — it’s about adopting a holistic approach that includes understanding your genetic background and making sustainable lifestyle changes.

My Best Heart Blood Pressure Support Supplement | 8 US Patents, 94+ Patent Claims | Cardiologist Developed | Red Spinach, Potassium Nitrates, Iron & Nitric Oxide Enzymes for Heart Health | 90 Capsules
8 US PATENTS & 99+ PATENT CLAIMS: My Best Heart is protected by 8 United States patents and…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Frequently Asked Questions
Can Hyperlipidemia Cause Symptoms Before a Heart Attack?
Hyperlipidemia often doesn’t cause early warning signs or noticeable symptoms before a heart attack. You might not realize your cholesterol levels are high until a serious event occurs. However, some people experience symptoms like chest pain, shortness of breath, or fatigue, which indicate underlying artery issues. Regular check-ups and blood tests are essential because symptom presentation can be subtle or absent until significant damage has happened.
Are There Natural Remedies to Lower Cholesterol Effectively?
They say “You are what you eat,” and that’s true for lowering cholesterol naturally. You can try herbal supplements like garlic or red yeast rice, which may help, along with dietary changes like eating more fiber, healthy fats, and reducing saturated fats. While these remedies can support your efforts, always consult with your healthcare provider to confirm they’re safe and effective for your needs.
How Often Should I Get Tested for Cholesterol Levels?
You should get a cholesterol screening every 4 to 6 years if you’re healthy and under 40. If you have risk factors like a family history or other health issues, your doctor may recommend more frequent blood tests. Regular blood tests help track your cholesterol levels and catch any problems early. Always follow your healthcare provider’s advice on blood test frequency to maintain your heart health effectively.
Is Hyperlipidemia Hereditary or Solely Lifestyle-Related?
Hyperlipidemia can be hereditary or influenced by lifestyle factors. You might have genetic factors that increase your risk, such as a family history of high cholesterol. However, lifestyle influences like diet, exercise, and weight also play a significant role. You can manage or reduce your risk by adopting healthier habits, but understanding your genetic predisposition helps you take targeted steps with your healthcare provider to control your cholesterol levels effectively.
What Are the Long-Term Risks of Untreated High Cholesterol?
If you leave high cholesterol untreated, you risk serious cholesterol complications like buildup in your blood vessels, leading to blockages. This can cause blood vessel damage, increasing your chances of heart attack, stroke, and peripheral artery disease. Over time, these issues can severely impact your health, so managing your cholesterol levels through lifestyle changes and medication is essential to prevent long-term damage and maintain your cardiovascular health.

Bell HDL Cholesterol Formulation™, Cholesterol Health Supplement – Unique Blend, for Women and Men | 30 Capsules
JUST ONE CAPSULE A DAY: HDL Cholesterol is a once-a-day capsule for your convenience, making it easier for…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Conclusion
Think of your arteries as a highway, and cholesterol as traffic. When too much cholesterol piles up, traffic jams happen, slowing everything down. I once knew someone who ignored their high cholesterol, and over time, it led to serious health issues. But with proper treatment and lifestyle changes, you can clear that traffic and keep your arteries flowing smoothly. Taking action now keeps your life’s highway running smoothly—don’t wait for a crash to make a move.

HOMEDSUN 4-in-1 Cholesterol Meter HSLPM-102 – Portable Blood Lipid Profile Analyzer Kit for TC, HDL, LDL, Triglycerides – Home Testing Device with 5Pcs Strips, Lancets, Droppers – Fast Results
Dedicated Support & 1-on-1 Guidance: Facing issues? Please contact us first! We offer personalized assistance to guide you…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.

Sunny Health & Fitness Smart Upright Row-N-Ride Exerciser, Squat Assist Trainer for Glutes Workout with Adjustable Resistance, Easy Setup & Foldable, Glute & Leg Exercise Machine- NO. 077S
【WHY WITH ROW-N-RIDE】Improve your squat form with this compact machine. Supports deeper range of motion while engaging the…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.